Spondylolisthesis
Spondylolisthesis
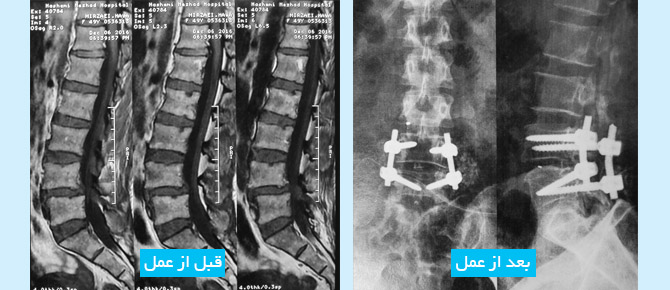
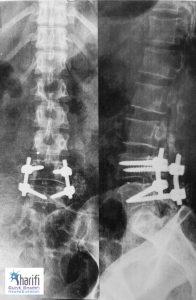
The patient was a woman with an L4-L5 lumbar spine problem. She suffered from severe pain in the leg and waist. Spinal cord decompression and vertebral fixation surgery were performed by Dr. Guive Sharifi (neurosurgeon). The operation was very satisfying and the patient gets well, thank God.
Preoperative Imaging
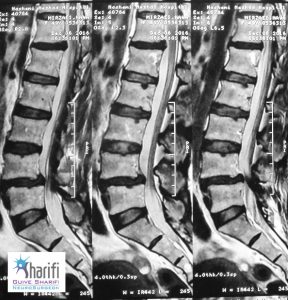
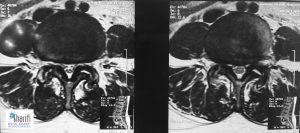
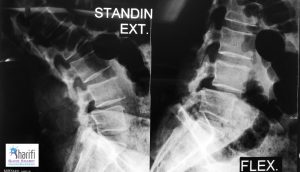
Postoperative Imaging