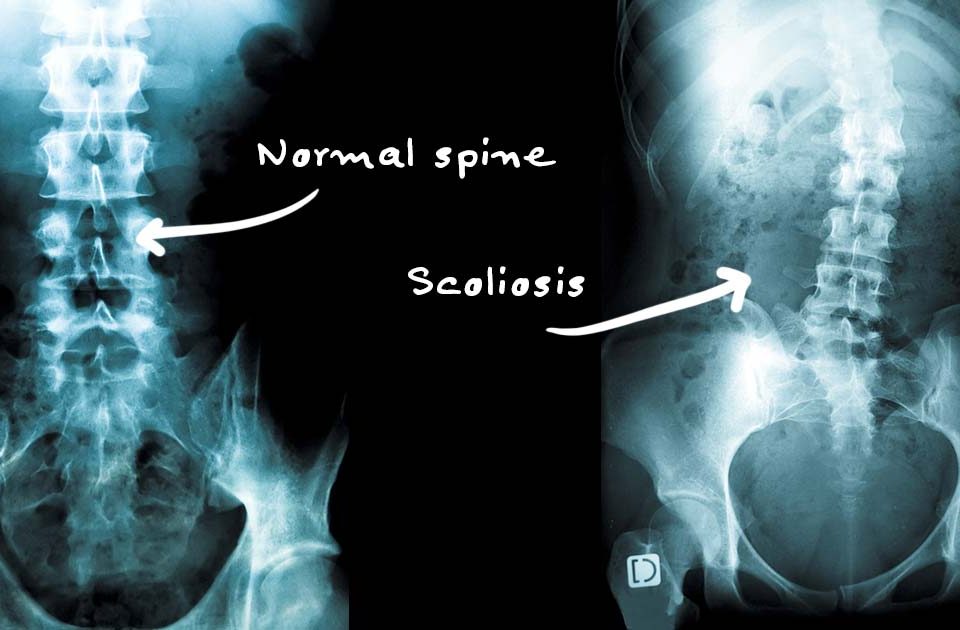
Osteoarthritis occurs when the protective cartilage in a joint begins to break down and no longer facilitates smooth movement between bones, which can eventually result in the joint becoming swollen and painful. When this condition develops in the cervical spine, it is called cervical osteoarthritis.
Sometimes confusion is created when general terms are used interchangeably to refer to cervical osteoarthritis, including cervical spondylosis, degenerative joint disease, or simply neck arthritis. On this site, cervical osteoarthritis is the term that specifically describes the degeneration of the facet joints in the cervical spine.
The Facet Joint and What Can Go Wrong
The facet joints, also called zygapophysial joints, are a key part of the spine’s flexibility. Two small facet joints are located at the back of each vertebral level (one to the right and one to the left), enabling limited forward/backward and twisting motion. In the cervical spine, these joints are called cervical facet joints.
A facet joint is comprised of hard yet smooth cartilage on the upper and lower articulating surfaces to protect the back part of vertebral bones. The joint is encased in a protective capsule, and inside this capsule is synovial fluid which provides the lubrication for smooth movements.
When the cartilage starts to wear away, bone starts rubbing against bone, which can facilitate excessive bone growth, known as bone spurs (osteophytes). Bone rubbing against bone can cause inflammation and pain. Furthermore, fragments of bone and cartilage might break off and start floating within the joint capsule’s synovial fluid, which can lead to more inflammation and discomfort.
Causes of Cervical Osteoarthritis
Cervical osteoarthritis becomes more common as people age, so the natural wear and tear sustained by the facet joints over time is considered to be a major factor in its development. However, the medical community continues to study the issue and other factors also appear to play a role in the development of osteoarthritis, including:
- Genetics. Some evidence suggests that osteoarthritis can run in families, which would indicate some people are genetically predisposed to having cartilage that breaks down sooner.
- Injury. If the joint becomes injured, such as a tear in the cartilage and/or protective joint capsule, the joint can become more inflamed and cartilage can wear down sooner. Joint injuries can happen in various ways, such as from a fall or while participating in a sport.
- Occupation. Certain occupations, such as jobs that involve lots of repetitive motions or heavy lifting like construction, can put more stress on the cervical spine.
- Weight. People who are overweight tend to develop osteoarthritis sooner, including in the neck. More weight means more stress on the joints, but another possibility could be that people with excess weight might experience more damaging inflammation.1
Cervical Discs
Normally, there are six gel-like cervical discs (one between each of the cervical spine’s vertebrae) that absorb shock and prevent vertebral bones from rubbing against each other while the neck moves. Each disc is comprised of a tough but flexible outer layer of woven cartilage strands, called the annulus fibrosus. Sealed inside the annulus fibrosus is a soft interior filled with a mucoprotein gel called the nucleus pulposus. The nucleus gives the disc its shock absorption property. Cervical degenerative disc disease is a common cause of neck pain and radiating arm pain. It develops when one or more of the cushioning discs in the cervical spine starts to break down due to wear and tear.
In children, the discs are about 85% water. The discs begin to naturally lose hydration during the aging process. Some estimates have the disc’s water content typically falling to 70% by age 70,1 but in some people the disc can lose hydration much more quickly.
As the disc loses hydration, it offers less cushioning and becomes more prone to cracks and tears. The disc is not able to truly repair itself because it does not have a direct blood supply (instead getting nutrients and metabolites via diffusion with adjacent vertebrae through the cartilaginous endplates). As such, a tear in the disc either will not heal or will develop weaker scar tissue that has potential to break again
Reference:
https://www.spine-health.com/conditions/arthritis/cervical-osteoarthritis-neck-arthritis
https://www.spine-health.com/conditions/degenerative-disc-disease/cervical-degenerative-disc-disease